By Iptisam Abdallah, Kakamega
Kenya records 22 neonatal mortality deaths per 1000 live births, a study has shown.
Urban areas have a higher rate of 26 deaths per 1000 live births compared to 21 deaths per 1000 births in the rural areas. On the other hand, maternal mortality stands at 590 deaths for 1000 live births since 1990.
Neonatal mortality refers to death of newborns in the first 28 days of life, with the earliest death occurring before 7 days and late deaths occurring between the 7th and 28th day whereas maternal mortality are the deaths of women that occur between pregnancy and childbirth.
A growing body of evidence suggests that stagnation of maternal and neonatal mortality in Kenya may be majorly caused by inability of health facilities to effectively manage delivery complications and sick newborns.
Kakamega County
Kakamega is among the counties that recorded high maternal and neonatal mortality rates as a result of inability of health facilities to effectively manage delivery complications and sick newborns. Delivery statistics show that only 37 percent of Kakamega county’s birth occur in a facility equipped to handle maternal emergencies.
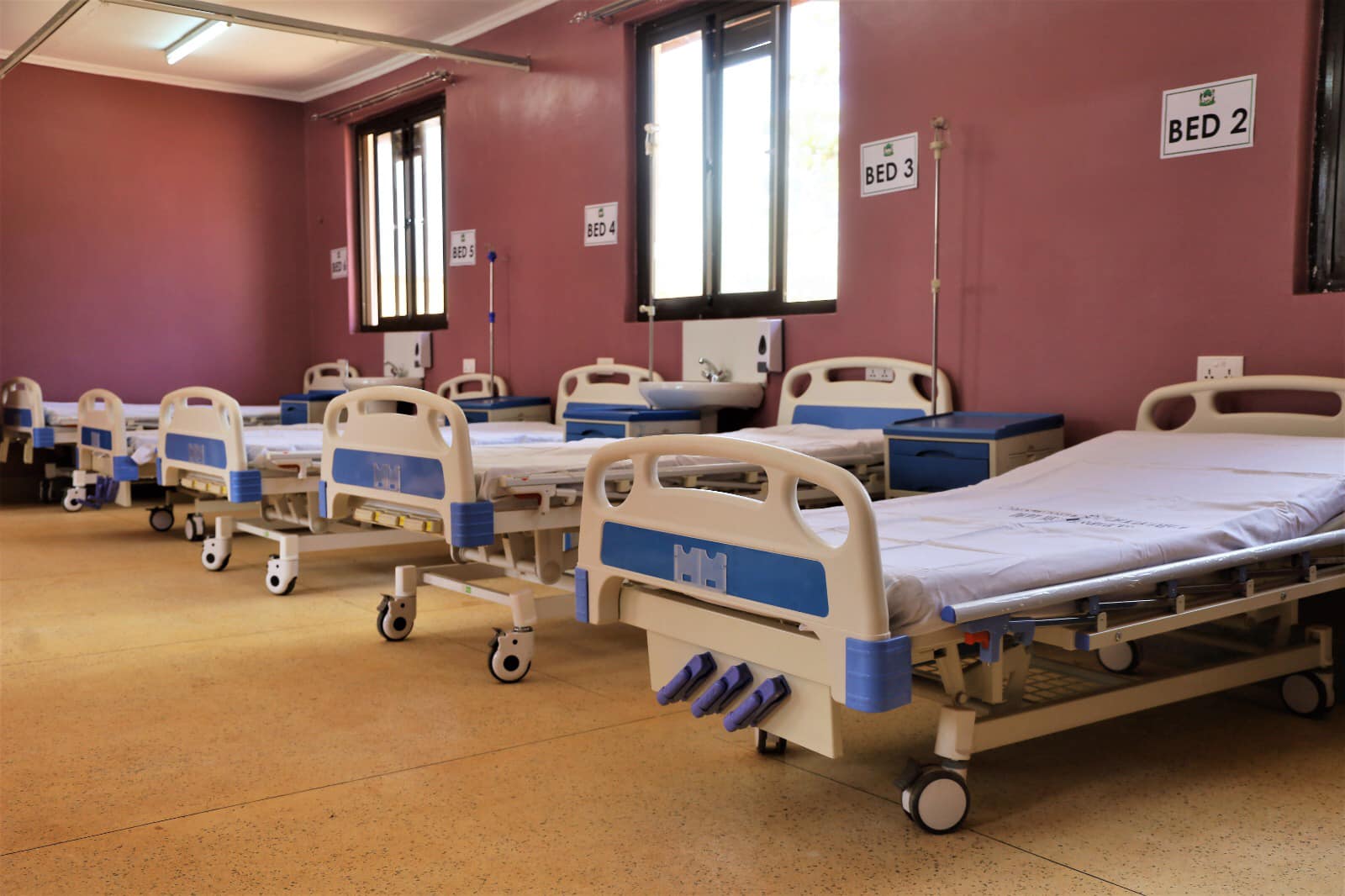
Deliveries were established to be sparsely distributed with 85 percent facilities conducting less than 30 deliveries per month. 99 percent of women in Kakamega live within 1 hour of advanced level 4/5 facility.
Tutunze Kakamega, Service Delivery Redesign
In attempts to reduce maternal and neonatal mortality rates, Kakamega County government with coordination with its health providers launched Tutunze Kakamega which is a cross sectional project that tests how to improve maternal and newborn survival by shifting where and when mothers access care.
Service Delivery Redesign focuses on improving the distribution of financing, staff, equipment, beds and medicine to ensure that women receive ‘right place, high quality care’ and mothers deliver in or as close as possible to well- functioning hospitals that are a comprehensive emergency obstetric and newborn care level 4/5.
Tutunze Kakamega project provides for expansion of the capacity of delivery services in hospitals to attend to deliveries and maternal and neonatal emergencies whilst improving the quality of antenatal and postnatal care in level 2 and 3 facilities. This will enable services such as screening, prevention and management of the growing burden of non-communicable diseases.
Investments will be made in urgent and emergency transportation and communication engagement,
ensuring no mother or community is left behind in accessing high quality health care.
Key components of Tutunze Kakamega Service Delivery Redesign
Since Kakamega county’s health system is overridden with problems including shortages of skilled medical officers and obstetricians capable of delivering timely, advanced and digified care to mothers, limited maternity bed-spaces critical hospital infrastructure, poor availability and coordination of affordable transport options, Jacaranda health providers collaborated with Build X Studio, Thinkplace, Thinkwell, Harvard University, John Hopkins University, Ipsos Synovate and KEMRI in generating replicable approaches and best practices for the provision of comprehensive and quality MNH care .
To mitigate the mentioned problems that impact the quality and sustainability of maternal health services accross the county, Tutunze Kakamega initiative provides for reasonable solutions.
This includes improving government health financing arrangements for quality health services and project sustainability through Thinkwell which works closely with the government in ensuring correct budgeting and strategic purchasing to ensure proper allocation of limited resources for the achieving significant outcomes for mothers and babies.
Through collaboration of the county government and Jacaranda Health, the initiative provides for high quality facilities for mothers. This will be possible through renovation of Lumakanda Hospital in Lugari Sub- County, extending the maternity wing of Malava hospital and construction of a new spacious hospital in Butere Sub- County.
The initiative also provides for increasing demand for high quality care by empowering over 70,000 to use Jacaranda’s digital platform called PROMPTS to safely navigate their pregnancies and connect to appropriate care in case of emergency.
Delays in receipt of care by urgent and emergency systems will be reduced through Rescue co’s ambulance dispatch service. This rescue team monitors location and distribution of public and private emergency vehicles. This service has enabled the evacuation of 500 mothers and babies under critical care. Through maximizing resources and real-time tracking of ambulances, the average response time has dropped from 1-3 hours to 29 minutes.
The initiative also provides for skilled providers to support mothers. This is done by training 50 healthcare workers in Emergency Obstetric and Neonatal care through Jacaranda’s peer to peer mentorship program called MENTORS.This nationally accredited program incorporates simulation drills and lectures to empower government providers to train providers in their respective facilities. The program also works to improve referrals by training providers in lower facilities to rapidly identify emergency cases in need of advanced care. Training 21 Emergency Medical Technicians and paramedics is also provided to ensure better quality care en-route to hospital.
Lastly, the initiative provides for uninterrupted access of blood and blood supplies in all delivery hubs. This is possible through the deployment of Jacaranda’s digital blood tracker across all 12 sub-counties of Kakamega. The blood tracker is actively used to request blood by unit, source and type during obstetric emergencies.
Expected Outcomes of Tutunze Kakamega Service Delivery Redesign
Tutunze Kakamega is expected to reduce the county’s maternal and Neonatal Mortality rate from 316/100000 and 19/1000 livebirths to meet a target of 7/100000 and 12/1000 in 5 years.
This project’s success will make Service Delivery Redesign to be adopted by stakeholders and county leadership as an evidence-based approach to resolving pain points across health system and increasing opportunities for legacy projects through capital expenditure.
End



